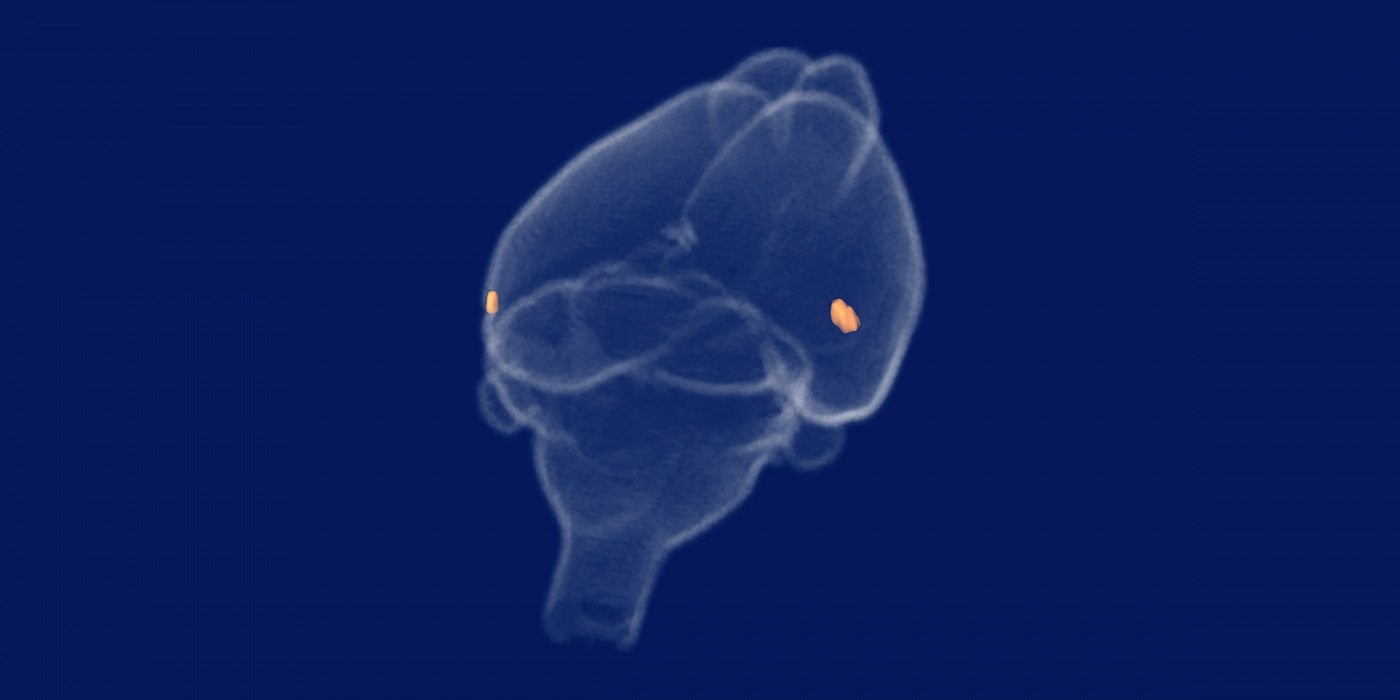
NEW YORK – When Alzheimer's disease first attacks the brain, it doesn't strike randomly. The damage tends to begin in the entorhinal cortex, a tiny hub especially connected to other parts of the brain. Why this area would be particularly vulnerable is a puzzle that scientists have been trying to work out for decades.
Researchers at Columbia University may finally have a solution, one that backs a new approach to developing treatments for this devastating neurodegenerative disease. Seven years of step-by-step sleuthing has implicated retromers: microscopic mail carriers that help package, ship and recycle molecules inside of cells. The scientists report their findings December 28 in Cell Reports.
“Efforts to treat Alzheimer’s disease have focused on what Dr. Alois Alzheimer observed more than a hundred years ago, but we have come a long way since then. Retromers offer a new direction and a new hope,” said Scott Small, MD, director of the Alzheimer’s Disease Research Center at Columbia University, the Boris and Rose Katz Professor of Neurology at Columbia University’s Taub Institute and Vagelos College of Physicians and Surgeons, and an affiliate member of Columbia’s Zuckerman Institute.
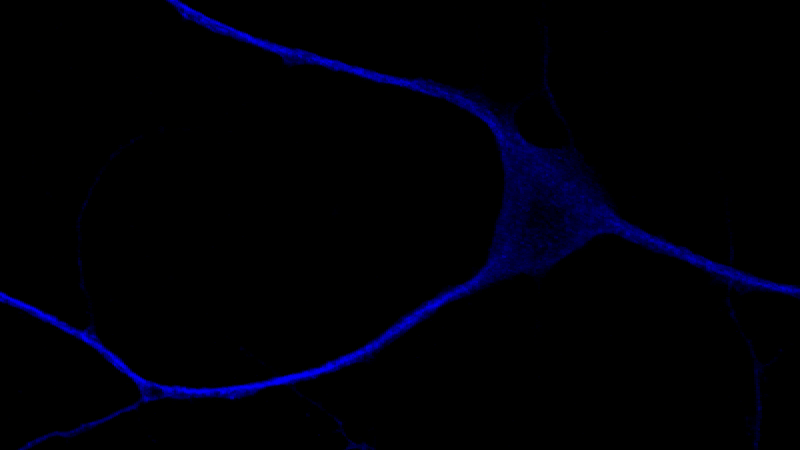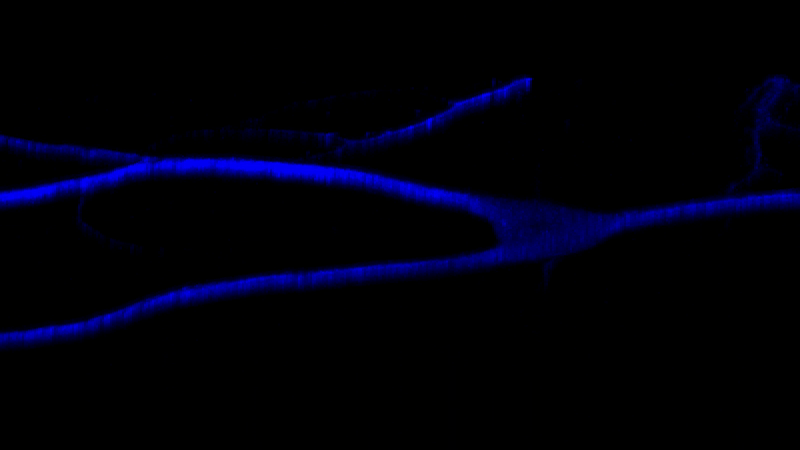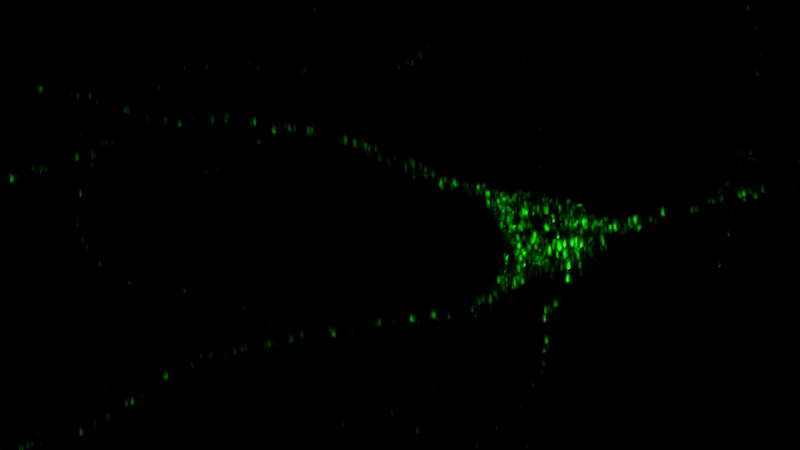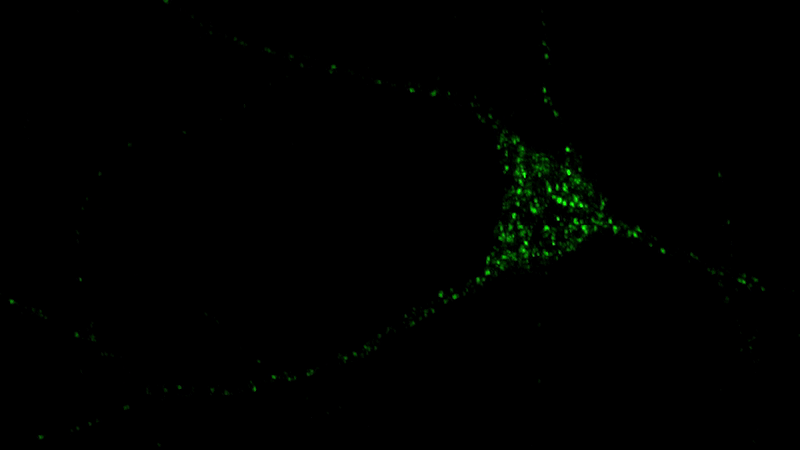
Shown here inside a neuron (blue), the retromer Vps26b (green) has emerged as a potential target for Alzheimer's disease (Credit: Sabrina Simoes / Small lab / Columbia University Irving Medical Center)
Starting with the Fundamentals
Sabrina Simoes, PhD, wasn't thinking about Alzheimer's when she first began exploring retromers as an associate research scientist in Dr. Small's lab. She had been reading about how, in organisms ranging from yeast to humans, every cell contains the retromer VSP26a. But only neurons, a type of brain cell, possess a different paralog of this retromer, VSP26b. As a scientist fascinated by the fundamental biology of cells, she found her curiosity piqued.
“I thought, 'This can't be a fluke, there must be some reason neurons need this second version of this retromer,'” said Dr. Simoes, who is now an Assistant Professor of Neurology at Columbia University’s Vagelos College of Physicians and Surgeons and Taub Institute. “So I took a closer look.”
Dr. Simoes grew and stimulated neurons in a dish. Under a microscope, she saw that the 26b paralog tended to hang out in cellular compartments used to recycle molecules inside brain cells: that is, to move molecules to and from the surfaces of neurons to regulate the cells’ electrical activity. The researcher wondered what role 26b plays in different brain regions. So she started working with mice from the University of Science & Technology in Korea that had been genetically modified to disable the Vps26b gene. And she teamed up with Jia Guo, PhD, an expert in the brain scanning technology functional magnetic resonance imaging at Columbia’s Zuckerman Institute.
Efforts to treat Alzheimer’s disease have focused on what Dr. Alois Alzheimer observed more than a hundred years ago, but we have come a long way since then. Retromers offer a new direction and a new hope.
A Surprising Scan
Dr. Guo used fMRI machines specially made for small animals to noninvasively scan the brains of the modified lab mice. He noticed something peculiar: a lack of activity in one small, sharply defined area in their brains, as compared to the brains of normal mice.
“I have never seen an fMRI imaging result in humans or other animals that was so striking, such a focused spot,” said Dr. Guo, an assistant professor in Columbia's Department of Psychiatry. “Normally, the differences in brain activity we see are fuzzy and diffuse.”
That spot coincided with a sliver of the entorhinal cortex brain region. When the researchers then directly measured the electrical activity of neurons in that area using electrodes, they found deficits, confirming the fMRI results. The mice also had trouble completing memory-related tasks known to involve the entorhinal cortex. Reintroducing working copies of Vps26b into the mice completely fixed these problems.
With all signs pointing to a link between the retromer and the entorhinal cortex, Simoes' fundamental cell biology work had been connected with Alzheimer's disease. That’s because neurological diseases have different hallmarks. Parkinson's starts in the substantia nigra, a brain region important for controlling the body. Huntington's first affects the striatum, related to rewards. And Alzheimer's, as has been known for decades, tends to set its sights on the entorhinal cortex.
“The evidence built up that this retromer variant, linked to cellular recycling, was crucial for proper brain function in the entorhinal cortex,” said Dr. Simoes. “This brain region's role in Alzheimer's led us to investigate whether the paralog could be related to the disease.”
Introducing SORL1
While the researchers were hard on the retromer's trail, another clue emerged. In 2007, a team that included Columbia’s Richard Mayeux, MD, MSc, chair of neurology at Columbia University Vagelos College of Physicians and Surgeons, had found a new gene connected to Alzheimer's. Mutations in this SORL1 gene were associated with late-onset Alzheimer's, which afflicts people over the age of 65, and SORL1 has emerged as one of the most damaging genes in the disease. Dr. Small and colleagues first found that the SORL1 protein is part of the same molecular shipping system associated with retromers.
Hoping to further connect this gene to their retromer variant, Dr. Small and his team checked their mice and found a deficiency of SORL1 in the entorhinal cortex. The scientists also examined brains donated by people diagnosed with Alzheimer’s and found a striking pattern: Tissues in the entorhinal cortex were depleted in both SORL1 and Vps26b.
Putting all these pieces together suggests that Alzheimer’s might begin with problems with a neuron’s ability to move molecules around. Scientists know the entorhinal cortex, a hub in the brain, forms an unusually large number of connections with other parts of the brain. These connections and the activity they generate could stimulate a lot of molecular recycling, making the entorhinal cortex especially susceptible to disruptions in these processes. For Dr. Small, these results hold promise for developing new treatments.
“Anchored in genetics and revealing that retromer dysfunction and SORL1 deficiency can explain the regional vulnerability we see in Alzheimer’s disease, this work validates the idea that retromer-enhancing drugs are worth pursuing for Alzheimer's disease therapeutics,” he said.
###
“Alzheimer’s vulnerable brain region relies on a distinct retromer core dedicated to endosomal recycling” appeared on December 28 in Cell Reports. Authors are Sabrina Simoes, Jia Guo, Luna Buitrago, Yasir H. Qureshi, Xinyang Feng, Milankumar Kothiya, Etty Cortes, Vivek Patel, Suvarnambiga Kannan, Young-Hyun Kim, Kyu-Tae Chang, Alzheimer’s Disease Neuroimaging Initiative, S. Abid Hussaini, Herman Moreno, Gilbert Di Paolo, Olav M. Andersen, and Scott A. Small.
The authors declare competing financial interests: Scott Small is a co-founder of Retromer Therapeutics, has equity in the company, and is a paid consultant to the company. In addition, Scott Small has equity in Imij Technologies, an MRI-based company. Gilbert Di Paolo is a full-time employee of Denali Therapeutics, Inc. Olav M. Andersen has commercial interests in Retromer Therapeutics. Lastly, Scott Small, Sabrina Simoes, and Yasir H. Qureshi are listed as co-inventors on Columbia University-owned patents that relate to retromer biomarkers and retromer drug discovery targets.
This study was partly supported by NIH R01 grants AG034618, AG035015, and P30AG066462 to S.A.S., NS056049 to G.D.P. and AG051556 to H.M. Human MRI data collection and sharing for this project were funded by the Alzheimer’s Disease Neuroimaging Initiative (ADNI) (NIH Grant U01 AG024904) and Department of Defense 409 ADNI (award number W81XWH-12-2-0012). Data collection and sharing for this project was partially funded by the ADNI (National Institutes of Health Grant U01 411 AG024904) and DOD ADNI (Department of Defense award number W81XWH-12-2-412 0012). ADNI is funded by the National Institute on Aging, the National Institute of Biomedical Imaging and Bioengineering, and through generous contributions from the following: AbbVie, Alzheimer's Association; Alzheimer's Drug Discovery Foundation; Araclon Biotech; BioClinica, Inc.; Biogen; Bristol-Myers Squibb Company; CereSpir, Inc.; Cogstate; Eisai Inc.; Elan Pharmaceuticals, Inc.; Eli Lilly and Company; EuroImmun; F. Hoffmann-La Roche Ltd and its affiliated company Genentech, Inc.; Fujirebio; GE Healthcare; IXICO Ltd.;Janssen Alzheimer Immunotherapy Research & Development, LLC.; Johnson & Johnson Pharmaceutical Research & Development LLC.; Lumosity; Lundbeck; Merck & Co., Inc.; Meso Scale Diagnostics, LLC.; NeuroRx Research; Neurotrack Technologies; Novartis Pharmaceuticals Corporation; Pfizer Inc.; Piramal Imaging; Servier; Takeda Pharmaceutical Company; and Transition Therapeutics. The Canadian Institutes of Health Research is providing funds to support ADNI clinical sites in Canada. Private sector contributions are facilitated by the Foundation for the National Institutes of Health (www.fnih.org). The grantee organization is the Northern California Institute for Research and Education, and the study is coordinated by the Alzheimer's Therapeutic Research Institute at the University of Southern California. ADNI data are disseminated by the Laboratory for Neuro Imaging at the University of Southern California.